Anesthesiology Understaffing Leads To Patient Deaths And Complications
Nikki Attkisson | Last Updated : July 23, 2022The research done by Sachin Kheterpal and colleagues from the University of Michigan found that insufficient anesthesiologist staffing practices do lead to increased surgical patient morbidity and mortality.
Anesthesia Risks Patient Deaths And Issues!!
Before moving further, let’s go through some terms clarification. The branch of medicine that provides relief from the pain before, during, or after the surgical procedure is anesthesiology. The medications administered are called anesthesia, and the doctors trained in this field are known as the anesthesiologist. And the terms can vary from country to country or continent to continent.
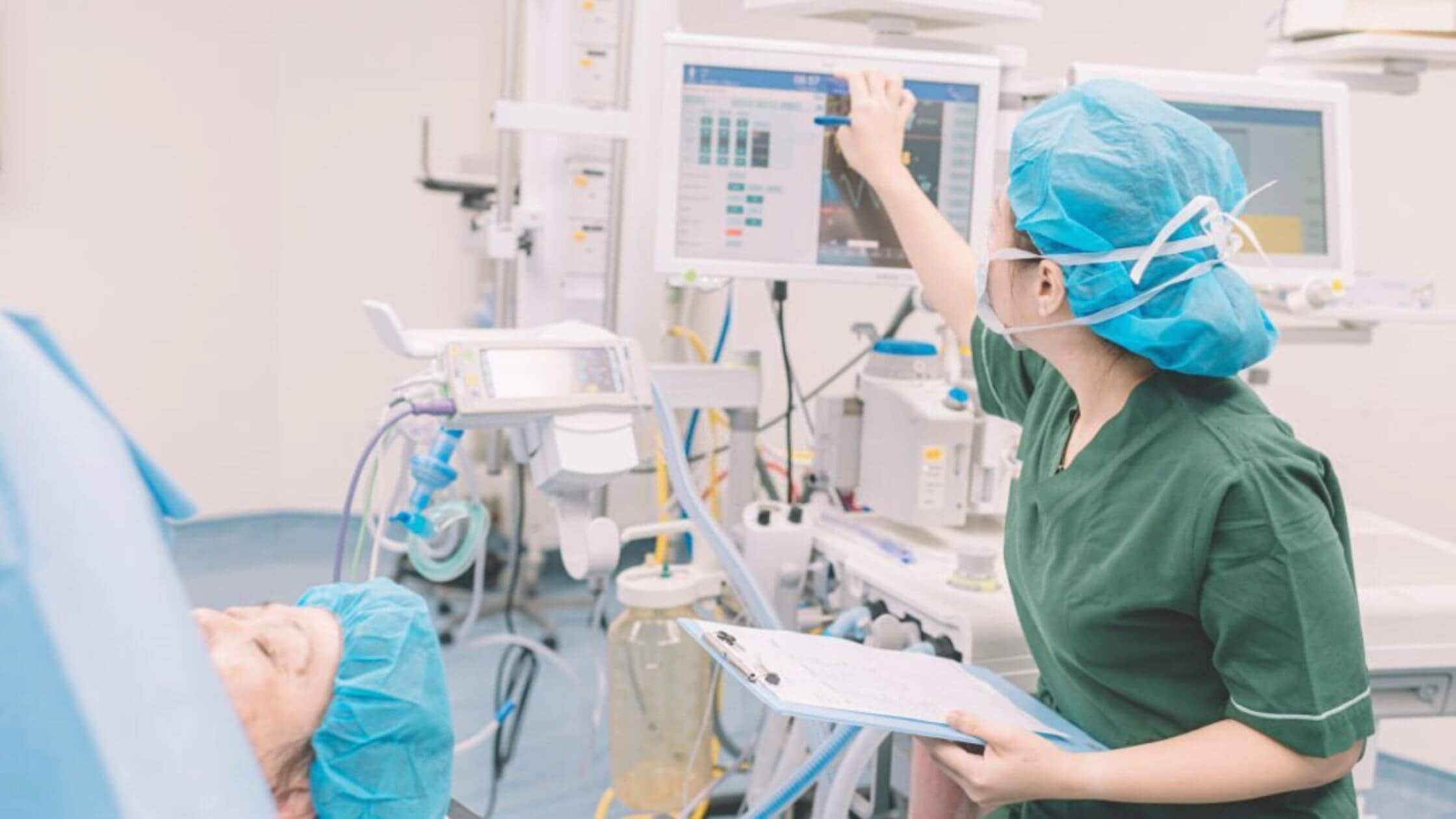
Sachin Kheterpal, MD, MBA, of the University of Michigan in Ann Arbor and the team reported that when the care teams had an anesthesiologist overseeing three to four overlapping surgeries instead of one or two, the morbidity and mortality rate of the risk-adjusted patient after 30 days was significantly higher.
And the respective rates also increase in teams with an anesthesiologist covering two or three overlapping operations (5.25%) rather than just one or two, the researchers documented in Jama surgery.
“Cost reduction measures usually target high fixed-cost anesthesiology services, considering that advanced clinical responsibilities are equivalent to lower patients to anesthesiologist staffing ratios”, reported the authors of the study. In addition, they wrote that comprehending the possible association with the grade of patient care is required to report clinical care staffing decisions.
The intricate process of anesthetizing a patient, temporarily making the patient unconscious, and removing sensation, is usually condescendingly referred to simply as turnover by surgeons, commented Martin Almquist, MD, Ph.D., of Skane University Hospital in Lund, Sweden.
He further continued, that the data collected displaying the number, skill, and experience of anesthesia staff is as highly crucial as surgeon competence, skill, volume, and experience for healthy outcomes.
Studies have found that nursing institutions with higher patient-to-nurse proportions have higher rates of all-around patient deaths. Increased physician clinical workload has decreased quality of care and poor clinical results.
There are various examples mentioned in the studies showing the deaths after complications, and other adverse effects and also of the internal medicine hospitalists and critical care intensivists wrote Kheterpal and co-authors.
Details of the study
The data was used from the Multicenter Perioperative Outcomes Group electronic health record registry for the study. The study was done on 578,815 patients who have undergone major noncardiac surgeries at 23 U.S. academic and private hospitals.
Patients were categorized as follows: Patients were categorized into four groups. The first group included 48,555 patients having an anesthesiologist covering one operation. The second group had 247,057 patients having two overlapping operations.
Group third contained 216,193 patients who had more than two to no more than three overlapping operations. 67,010 patients in the last group underwent four overlapping operations.
With disposition score matching, balanced sample groups regarding patient-, operative-, and hospital-level confounders were created.
The immediate overall outcome was 30-day mortality and the occurrence of six major surgical morbidities: cardiovascular, respiratory, gastrointestinal, hemorrhagic, infectious, and urinary complications.
After 30,026 operations, morbidity and mortality rate transpired and 30-day mortality surfaced after 2,607 operations. The complications occurred in the following ways:
- Respiratory after 6,645 operations
- Cardiac after 5,133 operations
- Gastrointestinal after 6,694 operations
- Urinary after 5,093 operations
- Bleeding after 4,457 operations
- Infectious after 4,963 operations
Bottom Line
The main limitation of the study was that a staff of a particular hospital observed might not depict all the clinical environments. Similarly, they recognized the possibility of unmeasured confounders, such as intraoperative patient acuity, the immediacy of operating rooms, and the stress level of the surgeon.
With over 15 years as a practicing journalist, Nikki Attkisson found herself at Powdersville Post now after working at several other publications. She is an award-winning journalist with an entrepreneurial spirit and worked as a journalist covering technology, innovation, environmental issues, politics, health etc. Nikki Attkisson has also worked on product development, content strategy, and editorial management for numerous media companies. She began her career at local news stations and worked as a reporter in national newspapers.
