Edoxaban May Help Treat Atrial Fibrillation After TAVI
Nikki Attkisson | Last Updated : September 1, 2021The ENVISAGE-TAVI AF study is the biggest to evaluate an edoxaban-based approach to anticoagulation, which really is presently the mainstay of therapy, in this client group. It proves that edoxaban isn’t worse than anticoagulation. The findings, which potentially lead to a new therapeutic approach, are presented as a late-breaking medical trial at the European Society of Cardiology’s 2021 Congress and concurrently posted in The New England Journal of Medicine on Saturday, August 28.
Edoxaban May Help Treat Atrial Fibrillation After TAVI
As per large-scale multinational research sponsored by Mount Sinai, the anticoagulant edoxaban could be just as efficient as warfarin in avoiding cardiac stroke or death in individuals with atrial fibrillation (AF) who have aortic valve restoration.
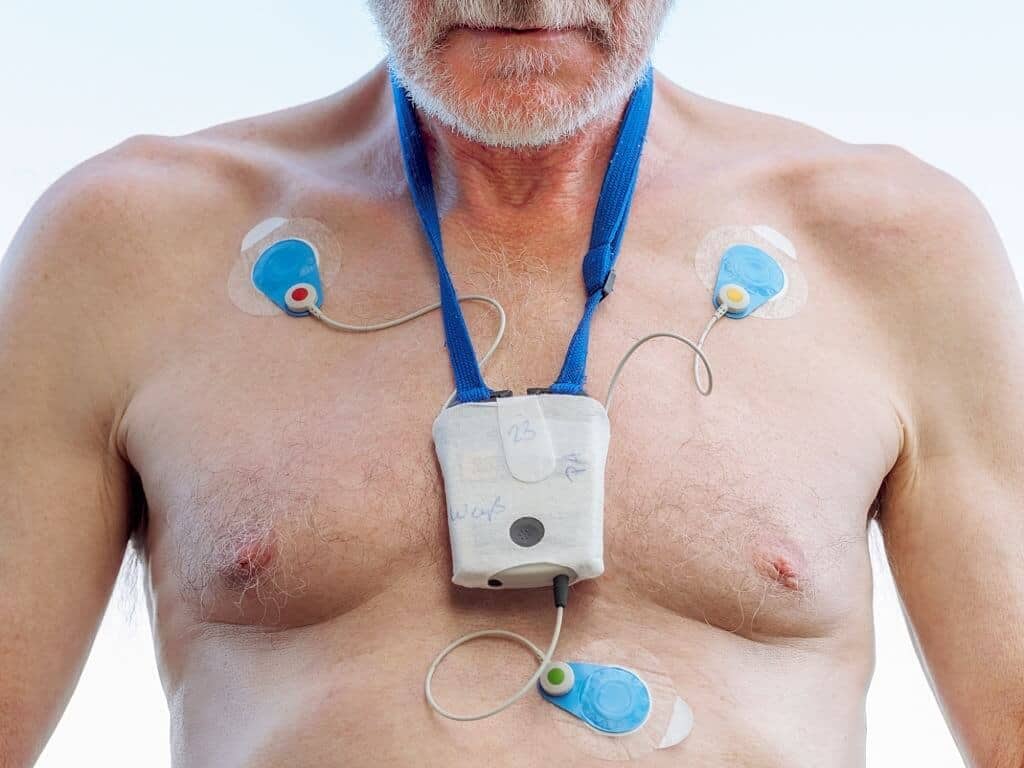
“Atrial fibrillation after transcatheter aortic valve replacement is common, especially among older patients, but there has been little research on the optimal treatment strategies, and this has resulted in heterogeneous use of anticoagulants in clinical practice. TAVR patients are typically very elderly and possess numerous comorbidities; therefore they are at high risk for all sorts of adverse events, both ischemic and bleeding.
Looking at their medical conditions the experts when they approach have left limited options. They have to face multiple conditions and TAVI can prove highly useful as it can easily handle the Arterial issues in the patient. This option has proven highly useful in a number of cases we have seen at our hospital one of the experts stated. We have made it a regular practice now. He added.
It is important to further understand what treatment is most effective to prevent devastating complications,” says lead investigator George Dangas, MD, Ph.D., Professor of Medicine (Cardiology) and Director of Cardiovascular Innovation at the Zena and Michael A. Wiener Cardiovascular Institute at the Icahn School of Medicine at Mount Sinai.
“Based on these results, the trial met its primary endpoint of non-inferiority and edoxaban may be a plausible alternative to warfarin, albeit with attention to increased bleeding with this agent in this study population.”
In AF individuals who require oral anticoagulation, Mount Sinai scientists launched a global trial involving 173 locations in 14 countries to examine the safety and effectiveness of edoxaban against warfarin. They examined all-cause death, thromboembolic outcomes, and significant hemorrhage as well as other adverse clinical events to establish efficacy.
They looked at significant hemorrhage occurrences for safety reasons. The researchers assigned 1,426 individuals to either warfarin or 60 mg daily administration of edoxaban 5 to 12 days following TAVR. Participants were kept upon for up to three years after TAVR.
In individuals who receive TAVR, a noninvasive heart treatment to repair the heart valve, cardiologists recommend antithrombotic medications, notably warfarin, a Vit D antagonist, to reduce thrombotic consequences. Selecting the best antithrombotic regimen can be difficult, particularly in patients who have an existing illness such as AF (abnormally fast heartbeat) that affects blood flow and necessitates the use of anticoagulants.
According to previous research, 20-40% of TAVR individuals have AF, and a high number of them are frail, therefore combining the dangers of hemorrhage and strokes is a major problem in monitoring their treatment.
“The next step would be to establish in large randomized trials the optimal anticoagulant dose according to different bleeding-ischemic risk profiles,” adds Dr. Dangas. “It seems that lowering the edoxaban dosage when indicated and avoiding patients with mandatory antiplatelet therapy because of their elevated bleeding risk is reasonable safety advice from the clinical point of view.
We will be conducting a detailed analysis of various types of bleeding in the near future. ENVISAGE-TAVI AF suggests that treatment with edoxaban can be valuable in the management of this high-risk population of AF patients after TAVI.”
With over 15 years as a practicing journalist, Nikki Attkisson found herself at Powdersville Post now after working at several other publications. She is an award-winning journalist with an entrepreneurial spirit and worked as a journalist covering technology, innovation, environmental issues, politics, health etc. Nikki Attkisson has also worked on product development, content strategy, and editorial management for numerous media companies. She began her career at local news stations and worked as a reporter in national newspapers.
