EPILEPSY: Genetic Risk Scores Help Diagnosis
Nikki Attkisson | Last Updated : September 1, 2021Henrike Heyne, MD (now at the Hasso Plattner Institute) and coworkers at the Research center for Molecular Medicine (FIMM) at the University of Helsinki, Finland, extracted data on 9660 people with epilepsy-related diagnoses and treatment from the over 269K persons would include in FinnGen venture and likened their polygenic threat ratings to that of control subjects. Those with seizures exhibited an increased genetic hazard for the illness, as anticipated.
EPILEPSY: Genetic Risk Scores Help Diagnosis
“In FinnGen we could also investigate the health records of participants who had suffered convulsions where the cause was unclear. Although some of them had later received a specific diagnosis of epilepsy, the majority had not. And we found that the genetic risk for epilepsy was significantly higher in individuals who received a specific epilepsy diagnosis than in those with only one seizure where the case was unclear,” says Dr. Heyne.
Among the top ailments that are dangerous for mass, the name of Epilepsy is at a very low rank but overall there are millions who suffer from this ailment worldwide. The majority of the causes are yet not known to experts which leads an individual to face it but the genetic disorder can be considered as one of the prime causes as many types of research have indicated the same at frequent intervals and with different samples.
While epilepsy is a prevalent disorder that affects about 1% of people globally, it can be hard to identify in medical care, and this is believed as close to a third of all instances are first misunderstood. Epilepsy is frequently hereditary, and a new study has revealed that patients have higher polygenic key metrics (PRSs) for the disorder.
PRSs may be used to help identify seizures in those who’ve had a solitary episode and differentiate them from others who have a seizure due to something else, according to Finnish researchers. The findings would be published today at the Euro Academy of Reproductive Genetics’ annual conference.
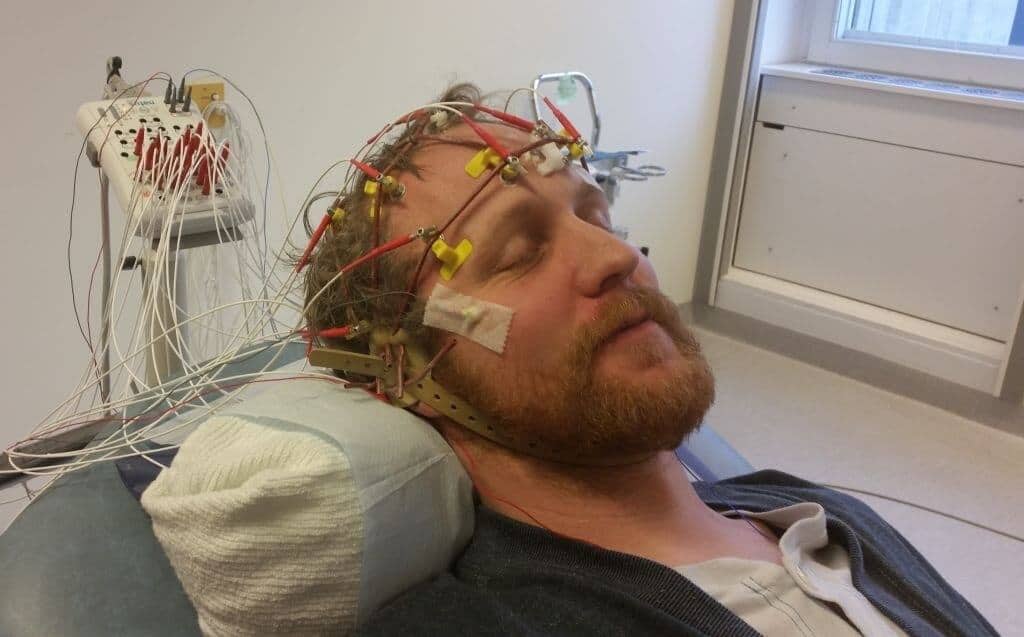
“In the future, genetic risk could be used as a biomarker for epilepsy,” adds Dr. Heyne. “This could be a great complement to existing techniques like electroencephalograms.” PRSs have been proved to be effective in a variety of disorders, and it is anticipated that their usage will be normal practice in the near, implying that genomic information may aid in the identification of epilepsy just following an episode.
The original study subjects varied in maturity from several weeks to over 90 years old. The scientists found that hereditary variables had a greater impact on people below the age of 40 than on those over 40.
This genetic component is especially strong in people with teenage myoclonic epileptic, which accounted for the majority of instances in the global epilepsy company’s current study of which gene mutations are associated with the greatest risk of epileptic seizures.
Despite the limited sample, the data clearly demonstrated the possibility for PRSs to be used in the prognosis, and the scientists expect to see them reproduced in larger trials which are more prevalent in other prevalent disorders like hypertension or diabetes.
Chair of the ESHG conference, Professor Alexandre Reymond, Director of the Center for Integrative Genomics, University of Lausanne, Lausanne, Switzerland, said: “Genetic information often tells us whether a person is at increased risk to develop a disorder or not. In this study, the authors have pioneered the use of a genetic risk score to identify people at risk for epilepsy.
Combining genetic data with other more traditional methods such as electroencephalograms could help the identification of epileptic individuals, potentially allowing early treatment. Of note is that about 25% of epilepsy patients are under an effective regimen.”
With over 15 years as a practicing journalist, Nikki Attkisson found herself at Powdersville Post now after working at several other publications. She is an award-winning journalist with an entrepreneurial spirit and worked as a journalist covering technology, innovation, environmental issues, politics, health etc. Nikki Attkisson has also worked on product development, content strategy, and editorial management for numerous media companies. She began her career at local news stations and worked as a reporter in national newspapers.
