Psoriatic Arthritis: Treatments Are Not Getting Better Results!
Nikki Attkisson | Last Updated : July 30, 2022When one aspect of the disease appears under control, another one can suddenly appear, making it difficult to manage a chronic condition like psoriatic arthritis (PsA). Psoriatic arthritis (PsA) is a musculoskeletal condition that is persistent, inflammatory, and related to psoriasis.
Psoriatic Arthritis: Confidence Is The Only Solution!
PSA can occur in up to 30% of psoriasis sufferers throughout the course of their lives. As people look for symptom relief to assist enhance well-being, which can encompass physical and emotional health, this may frustrate medical professionals and their patients.
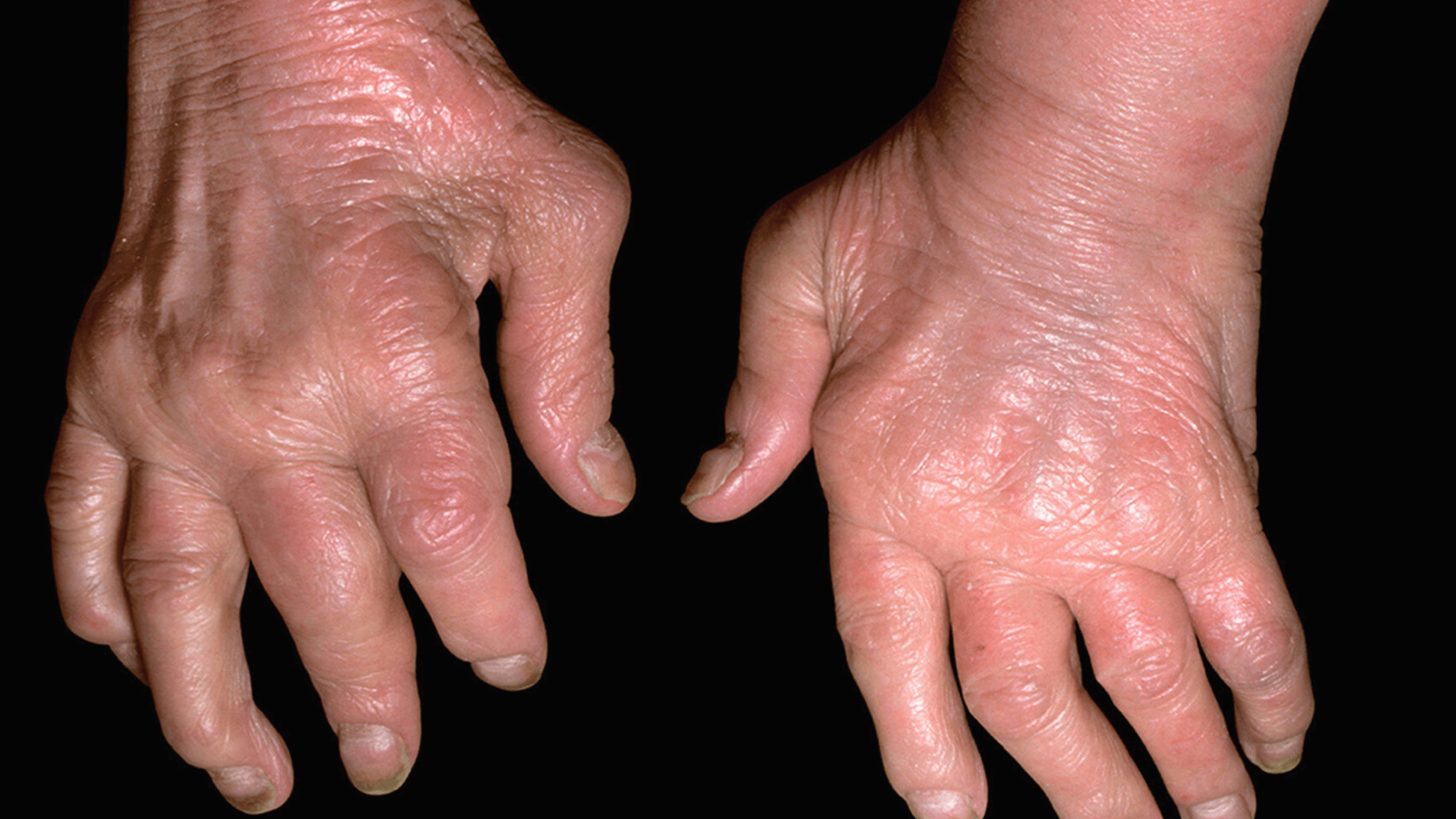
Many PSA patients may be dissatisfied with how the disease affects their ability to perform daily tasks or how they are responding to treatment. For instance, if they experience short-term symptomatic relief but not long-term symptomatic relief, due to the unpredictable nature of PsA, an immune-mediated disease that is frequently debilitating and characterized by swollen joints and stiffness.
Many patients get used to the ups and downs of their painful symptoms and times when they feel better. However, those who have PsA deserve better. They deserve to know how to manage their PsA holistically and uniquely, to help them manage their symptoms, slow the course of the disease, and feel their best.
Peripheral arthritis, spondylitis, dactylitis (inflammation of the entire digit), and enthesitis are musculoskeletal symptoms of PsA (Inflammation of the area where a tendon, ligament, or joint capsule inserts into the bone). Psoriasis (which has many phenotypes but the most typical kind associated with PsA is psoriasis Vulgaris or plaque psoriasis) and nail disease are examples of skin manifestations of PsA. Patients with PsA report fatigue, physical function limits, sleep disturbance, as well as reduced work capability and social participation, in addition to musculoskeletal and skin symptoms.
PSA is linked to a number of comorbidities, including obesity and metabolic disease (diabetes, hypertension, hyperlipidemia, fatty liver disease, cardiovascular consequences), depression, and anxiety, in addition to extra-articular symptoms such as uveitis and inflammatory bowel disease (IBD). Patients with PsA have more comorbidities than the general population, with more than half of patients having at least one comorbidity in addition to the consequences of the disease itself.
Science is developing at the same time as this improvement in comprehensive disease management. Patients can choose from a number of treatments to relieve symptoms like pain, stiffness, and inflammation. These medications include biologics, disease-modifying antirheumatic medicines, and non-steroidal anti-inflammatory drugs. Additionally, certain biologic medications have clinical data supporting their ability to reduce fatigue symptoms.
As a result, there is a chance to provide patients with more options, which is crucial given that PsA is a chronic condition that has no known treatment. It’s vital to assist patients to understand that it might take time to find the proper treatment plan, and it’s not a failure if adjustments need to be made over time. PSA severity can vary from patient to patient, symptoms may feel invisible and be difficult to define, and it’s a progressive disease. In order to better adapt their treatment plan to meet their unique needs, patients and clinicians can have an open discussion about what is and isn’t working, from medication and lifestyle changes to techniques that improve mental and emotional wellness.
Existing therapy recommendations have their limits, and complicated, heterogeneous illness guideline development requires new approaches. There isn’t a single best recommendation made for all clinicians. Society may endeavor to make feeling just “ok” or “good enough” a thing of the past as people better comprehend the entire range of PsA symptoms and as more treatment choices become accessible. It’s time to give PsA sufferers the confidence to demand more of themselves and to place a higher priority on their general well-being.
With over 15 years as a practicing journalist, Nikki Attkisson found herself at Powdersville Post now after working at several other publications. She is an award-winning journalist with an entrepreneurial spirit and worked as a journalist covering technology, innovation, environmental issues, politics, health etc. Nikki Attkisson has also worked on product development, content strategy, and editorial management for numerous media companies. She began her career at local news stations and worked as a reporter in national newspapers.
